Imagine the stress of relying on a life-saving medication, only to have your body treat it like an enemy. For most people with diabetes, insulin is a routine part of the day. But for a small group, the injection site becomes a battleground of redness, itching, or even systemic distress. While insulin allergies are rare, they can be terrifying because you can't simply stop taking the medicine without risking a metabolic crisis.
If you've noticed a bump that won't go away or a rash after your dose, you aren't alone. About 2.1% of people with diabetes deal with some form of immune-mediated reaction to insulin. The good news is that these reactions are manageable, and you don't have to just "live with the itch." Understanding whether you're dealing with a local skin issue or a full-blown systemic allergy is the first step toward getting your skin-and your peace of mind-back.
The Quick Breakdown: Local vs. Systemic Reactions
Not all reactions are created equal. In fact, the vast majority of insulin allergies-around 97%-are localized. This means the trouble stays right where the needle went in. However, a tiny fraction of users experience systemic reactions, where the immune response travels through the bloodstream to affect the whole body.
Localized reactions usually start as redness, swelling, and itching. If left alone, these can turn into tender subcutaneous nodules (hard lumps under the skin) anywhere from 30 minutes to 6 hours after your shot. On the other hand, a systemic reaction is an immediate, full-body alarm. This can include hives, a widespread rash, or angioedema (deep swelling under the skin). In the rarest and most dangerous cases, this leads to anaphylaxis, where your blood pressure drops and your airway narrows.
| Feature | Localized Reaction | Systemic Reaction |
|---|---|---|
| Frequency | Common (approx. 2-3% of users) | Very Rare (< 0.1% of users) |
| Key Symptoms | Redness, itching, hard nodules | Hives, swelling, difficulty breathing |
| Onset Time | 30 minutes to 6 hours | Immediate |
| Urgency | Schedule doctor visit | Emergency room/999/911 |
Is it an Allergy or Something Else?
It's easy to confuse a true allergy with other common insulin side effects. For example, feeling shaky, sweaty, or anxious is usually a sign of hypoglycemia (low blood sugar), not an allergic reaction. Similarly, a small bruise at the injection site is often just mechanical trauma from the needle, not an immune response.
A true Insulin Allergy is an adverse immune-mediated reaction to the insulin molecule or its added ingredients. Most of these are IgE-mediated, meaning your body produces specific antibodies that trigger the reaction. However, some people experience a delayed hypersensitivity. This is a T-cell mediated response that can happen 2 to 24 hours after the shot, often resulting in bruising or joint pain (arthralgia). Interestingly, some people develop this delayed reaction even after using the same "human" insulin for a decade without any issues.
Another twist is that you might not be allergic to the insulin itself. Many insulin formulations contain metacresol, a preservative that helps keep the medication stable. Some patients react specifically to this excipient or to the zinc used in the formula. For instance, certain fast-acting insulins like Humalog have higher concentrations of metacresol, which might make them more irritating for sensitive individuals.
How Doctors Diagnose the Reaction
You can't diagnose an insulin allergy by just looking at a rash; you need an allergist to get a clear picture. The process usually starts with a detailed history-when does the reaction happen? How long after the shot? Which brand of insulin are you using?
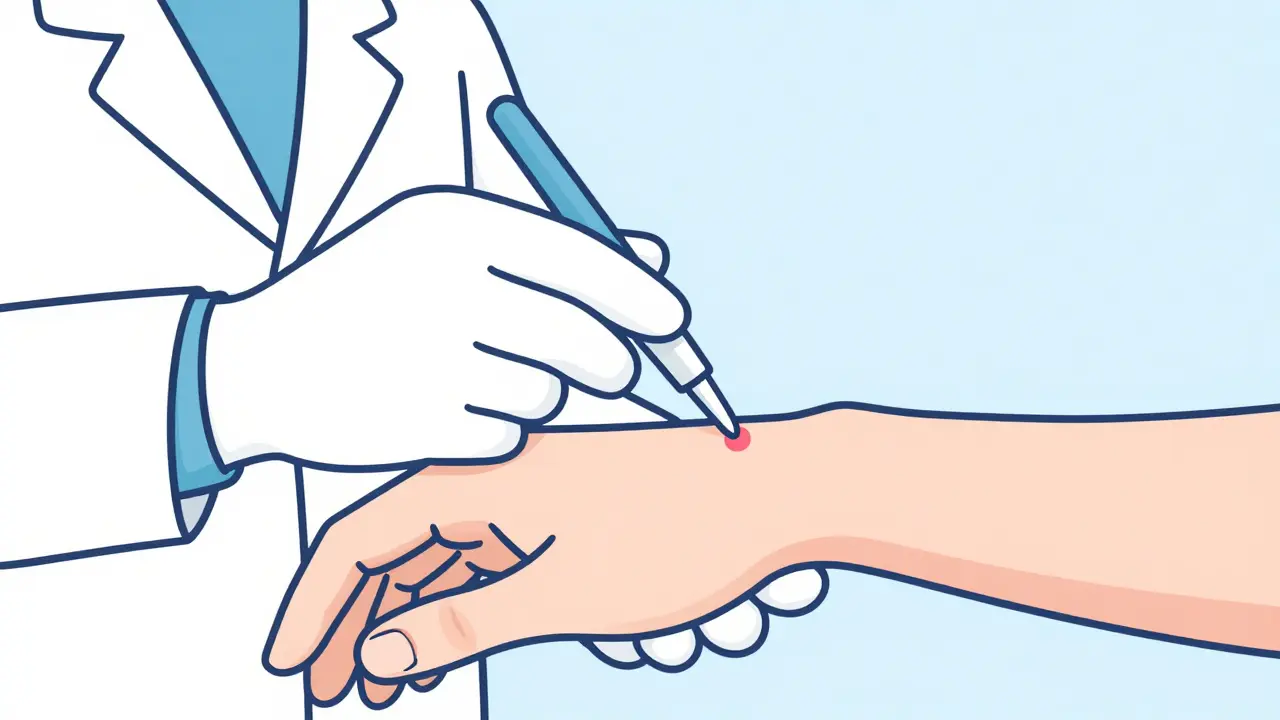
The gold standard for diagnosis involves Skin Prick Testing. The doctor places a tiny amount of the suspected insulin on your skin and pricks it slightly to see if a "wheal" (a small bump) forms. If that's inconclusive, they might move to intradermal testing or blood tests to measure specific IgE antibodies. This tells the medical team exactly what the trigger is: the insulin protein, the preservative, or something else entirely.
Managing the Itch and Swelling
The most important rule is this: Do not stop taking your insulin without talking to your doctor. If you have Type 1 diabetes, stopping insulin can lead to diabetic ketoacidosis (DKA) very quickly, which is far more dangerous than a skin rash.
For mild localized reactions, the first line of defense is usually antihistamines to stop the itching and steroids to calm the inflammation. If you're dealing with the delayed, T-cell mediated response, experts suggest using calcineurin inhibitors like tacrolimus or pimecrolimus. Applying these topically right after the injection and again 4-6 hours later can suppress the skin's reaction.
If topical creams aren't enough, some patients find success with mid-to-high potency corticosteroids, such as flunisolide 0.05%. The key is consistency-applying it immediately and then again a few hours later prevents the reaction from gaining momentum.
Advanced Treatments and Long-Term Solutions
When basic creams and pills don't work, doctors move to more systemic strategies. One of the most effective methods is switching the type of insulin. Because different brands use different purification processes and excipients, switching can resolve the issue for about 70% of patients.
For those who still react after switching, Specific Immunotherapy (desensitization) is an option. This involves giving the patient gradually increasing doses of the insulin they are allergic to. It sounds counterintuitive, but it essentially "trains" the immune system to tolerate the protein. Research shows that about 66.7% of patients see their symptoms disappear completely with this method.
In very rare cases, specifically for those with Type 2 diabetes who can tolerate it, doctors may transition the patient to oral antidiabetic medications to remove the need for injections entirely. However, this is not an option for those with Type 1 diabetes.

When to Call 999 or 911
While most reactions are just annoying, a systemic allergic reaction can be fatal if not treated. You need to seek emergency medical help immediately if you experience any of the following after an injection:
- Swelling of the lips, tongue, mouth, or throat.
- Difficulty breathing or wheezing.
- A sudden drop in blood pressure (feeling like you might faint).
- Rapidly spreading skin discoloration or hives across the body.
In these scenarios, don't try to drive yourself to the hospital. Call emergency services. Anaphylaxis requires immediate intervention with epinephrine and professional monitoring to keep the airway open.
Can I develop an insulin allergy after years of using it?
Yes. While many allergies start immediately, delayed hypersensitivity reactions can develop even after 10 years or more of using human insulin. This is often a T-cell mediated response rather than a sudden IgE reaction.
Does switching brands always work?
It works for approximately 70% of people. The success depends on whether you are reacting to the insulin molecule itself or to a specific preservative (like metacresol) that might be present in one brand but not another.
What is the difference between a local reaction and a side effect?
A local reaction is an immune response involving redness, itching, and swelling. A side effect, like sweating or trembling, is usually a physiological response to the insulin's effect on your blood sugar (hypoglycemia), not an allergy.
How does desensitization work for insulin?
Specific immunotherapy involves administering tiny, gradually increasing doses of the insulin protein. This process helps the immune system stop recognizing the insulin as a threat, which can lead to a complete resolution of symptoms in many patients.
Can preservatives cause these reactions?
Absolutely. Many people aren't allergic to the insulin itself but to excipients like metacresol or zinc. Because different brands use different concentrations of these additives, switching brands often helps.
Next Steps for Your Care
If you suspect you have an allergy, start a "reaction log." Note the exact time you injected, the brand of insulin used, the site of the injection (thigh, abdomen, arm), and exactly when the symptoms started. This data is gold for your doctor.
Your next move should be a joint consultation. A diabetologist manages your glucose, but an allergist manages your immune system. For the best results, these two specialists need to coordinate your treatment-especially if you are starting immunotherapy, as your blood sugar may need tighter monitoring during the process.



Anastasios Kyriacou
April 23, 2026 AT 10:23just swap brands mate, easy fix for most ppl
Ajinkya Joshi
April 24, 2026 AT 22:03Oh wow, a chart. How revolutionary. I'm sure the 0.1% of people having a systemic reaction are thrilled that we've categorized their near-death experience into a neat little table for the internet to enjoy
Amy Fredericks
April 26, 2026 AT 10:48It's so important to remember that everyone's journey with diabetes is different. If you're struggling with these reactions, please know there are solutions and you don't have to face it alone!
RAJESH MARAVI
April 28, 2026 AT 03:21idk why evryone trust these gudes... my cousin used a diff brand and still got lumps!! these stats are probly fake news anyway
Caroline Duvoe
April 29, 2026 AT 14:23already knew about the metacresol thing 🙄 just a basic chemistry issue really 💅
Sue Stoller
April 30, 2026 AT 05:37You've got this everyone! ✨ Just keep tracking those reactions and stay positive while working with your doctors! 💖🌈
Mike Arrant
May 1, 2026 AT 08:25You're probably just injecting into the same spot too often. Stop being lazy with your rotation and the bumps will go away. Most people just don't have the discipline to rotate properly.
Mayur Pankhi Saikia
May 1, 2026 AT 13:31The lack of depth here is... appalling...!! One must consider the biochemical variance in protein folding before simply suggesting a "brand switch"...!! Truly amateurish observations...!!
Dave Edwards
May 3, 2026 AT 08:03The audacity to suggest desensitization as a primary path! It's practically torture to inject something you're allergic to just to "train" the body! Absolute madness 😱
Saptatshi Biswas
May 4, 2026 AT 05:35This is exactly why Indian pharmaceutical standards are superior to the Western garbage mentioned here. We prioritize precision over profit in our formulations, and the systemic failure of US healthcare is glaringly obvious in these rare reaction rates!
Emma Cozad
May 5, 2026 AT 06:28USA made insulin is the only thing keepin people alive while other countries just guess. This whole post is just tryin to make it sound scary for no reason lol
Mel Glick
May 5, 2026 AT 07:32I totally agree with the part about the reaction log. If you aren't tracking your sites, you're basically guessing. Get a notebook and do the work or stop complaining about the itch!
vimal purwal
May 5, 2026 AT 21:54I would like to most emphatically concur with the necessity of the joint consultation mentioned at the end of the text, as the synergy between a diabetologist and an allergist is paramount for patient safety and optimal glycemic control, and I believe that failing to coordinate these two specialties can lead to suboptimal outcomes for the patient in the long run.
Odicha ude Somtochukwu
May 7, 2026 AT 01:34It is truly heartening to see such comprehensive guidance provided for those in need...!! May we all find the strength to manage our health with grace and patience...!! God bless you all...!!
Nicole Antunes
May 7, 2026 AT 05:51I've seen a few people in my support group use the topical steroids mentioned, and they've had wonderful results. It's just so helpful to have a clear path forward when you're feeling overwhelmed by a new symptom. Keep supporting each other, everyone! :)