Every year, over 200,000 adverse events linked to sedatives and opioids happen in U.S. healthcare settings. Seniors make up 65% of the cases where breathing stops completely during procedures. Why? Because aging changes how the body handles medicine. The liver slows down. Kidneys filter less. The brain becomes more sensitive. A dose that’s safe for a 40-year-old can push an 80-year-old into respiratory arrest. Monitoring isn’t optional-it’s the line between life and death.
What Over-Sedation Looks Like in Seniors
- Slowed breathing - Less than 8 breaths per minute. This is the most dangerous sign. Many seniors on oxygen won’t turn blue right away. Their SpO2 stays above 94%, but they’re not moving air. That’s called silent hypoxia.
- Unresponsiveness - If you shake their shoulder and they don’t open their eyes or grunt, they’re too deep. The Richmond Agitation-Sedation Scale (RASS) scores this. A score of -3 or lower means moderate to deep sedation. At -5, they’re unarousable. That’s an emergency.
- Low blood pressure - Systolic pressure below 90 mmHg. Sedatives relax blood vessels. In seniors, that can crash their heart’s ability to pump.
- Heart rate changes - Below 50 or above 100 beats per minute. Either extreme signals trouble. A slow heart rate often means the brain is shutting down from lack of oxygen.
- Confusion or agitation - Sometimes, oversedation looks like the opposite: sudden restlessness or yelling. This isn’t dementia flare-up. It’s the brain struggling to process what’s happening.
These signs don’t always show up together. One nurse at Mayo Clinic told me about an 89-year-old who looked fine-eyes open, breathing regular-until her capnography alarm went off. Her CO2 levels had climbed to 68 mmHg. She was holding her breath. No one noticed because she was on oxygen.
The Monitoring Tools That Save Lives
Don’t rely on checking pulse oximetry every 10 minutes. That’s like checking your car’s oil once a week while driving on the highway. You need continuous, multi-parameter monitoring.
- Capnography - This measures carbon dioxide (EtCO2) in exhaled breath. Normal is 35-45 mmHg. If it drops below 30 or rises above 50, it’s a red flag. In seniors on oxygen, capnography catches breathing problems 12-14 minutes before pulse oximetry does. It’s not perfect-irregular breathing in COPD patients causes false alarms-but it’s still the gold standard.
- Pulse oximetry - SpO2 should stay above 92%. Alarms should trigger at 90%. But remember: if a senior is on supplemental oxygen, their SpO2 can look normal even if they’re barely breathing. Capnography catches what oximetry misses.
- Integrated Pulmonary Index (IPI) - This is a single number (1-10) that combines heart rate, breathing rate, SpO2, and EtCO2. A score below 7 means intervention is needed. In a 2021 study of 1,245 elderly patients, IPI predicted respiratory failure 12.7 minutes before oxygen levels dropped. One nurse on Reddit described how her 82-year-old patient’s IPI dropped to 5.2 during a colonoscopy. They paused the procedure. The patient woke up. No harm done.
- Respiratory Volume Monitoring (RVM) - Uses bioimpedance to measure actual air movement. It’s better than capnography for detecting shallow breathing. But electrodes often fall off on fragile elderly skin. Use hydrocolloid dressings underneath to keep them stuck.
- ECG and NIBP - Continuous heart rhythm and non-invasive blood pressure checks are mandatory. Heart rate under 50 or systolic BP under 90? Stop the procedure. Assess immediately.
There’s no single tool that does it all. Capnography + pulse oximetry is the minimum. Add IPI or RVM if you can. Anything less is gambling.
Medication Dosing: One Size Does NOT Fit All
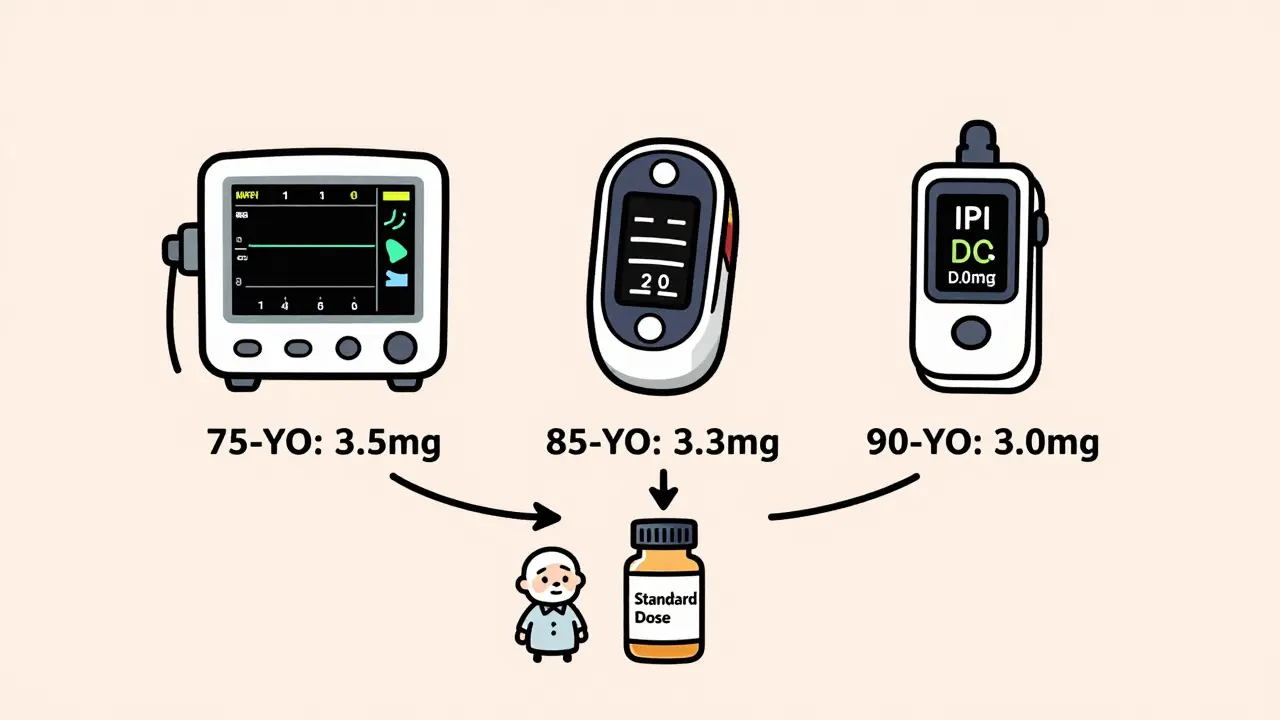
Doctors still give seniors the same opioid or sedative doses as healthy 30-year-olds. That’s dangerous. Here’s the math: for every year over 60, reduce the dose by 0.5%. So a 75-year-old should get 7.5% less than the standard dose. A 90-year-old? 15% less.
Formula: Dose = Standard Dose × (1 - 0.005 × (Age - 20))
Example: Standard midazolam dose is 5 mg. For an 85-year-old: 5 × (1 - 0.005 × 65) = 5 × (1 - 0.325) = 5 × 0.675 = 3.375 mg. Round to 3.5 mg.
And never assume. Even if the chart says “no allergies, no liver disease,” seniors metabolize drugs differently. Always start low. Go slow. Wait 5 minutes after each dose. Watch the monitors.

Common Mistakes That Kill
- Assuming oxygen masks mean safety - A mask keeps SpO2 high, but doesn’t stop CO2 buildup. That’s why capnography is non-negotiable.
- Ignoring RASS scores - If a patient is at -4 (deep sedation), they’re not “just sleeping.” They’re one breath away from arrest. Intervene.
- Missing COPD patterns - Seniors with chronic lung disease often have wavy, irregular capnography waveforms. Don’t mistake that for a machine error. Learn the difference between a normal COPD pattern and a dangerous one.
- Alarm fatigue - Nurses get used to beeping machines. 47% of capnography alarms in seniors are false. But 127 documented over-sedation cases in 2023 were caused by ignoring alarms. Train staff to respond to every alert, even if it’s “probably wrong.”
- Using intermittent checks - Checking vitals every 5 minutes misses 78% of respiratory events. Continuous monitoring isn’t luxury-it’s the standard.
What Facilities Are Doing Right
At Mayo Clinic, they combined continuous capnography with RASS scoring for patients over 75. Result? A 41% drop in oversedation events. At Johns Hopkins, they automated dose calculations into their EHR. Nurses input age and weight. The system suggests adjusted doses. Error rate dropped 63%.
Outpatient endoscopy centers lag behind. Only 28% use continuous capnography. That’s where most senior overdoses happen. If you’re running one, start here: install capnography. Train staff on RASS. Use the dose formula. You’ll cut risk by half.
What to Do If You See Warning Signs
Here’s your action plan:
- Stop the procedure - Immediately pause any sedation delivery.
- Call for help - Get a second nurse, an anesthesiologist, or a code team.
- Remove oxygen mask - If they’re on it, take it off. You want to see their natural breathing pattern.
- Give naloxone - If opioids are involved, give 0.4 mg IV. Repeat every 2-3 minutes if no response. Don’t wait for confirmation. If you suspect overdose, act.
- Bag-mask ventilation - If breathing stops, use a bag-valve mask. Deliver 1 breath every 5-6 seconds.
- Monitor for 1 hour - Even after they wake up, keep watching. Re-sedation can happen hours later.
Final Reality Check
Technology helps. But no monitor replaces a trained human watching closely. The 2023 NCEPOD report found that 28% of monitoring failures happened because staff trusted the machine too much. One case: a patient’s SpO2 read 87-91% for 12 minutes. Staff thought it was “normal fluctuation.” The patient coded.
Monitoring seniors isn’t about gadgets. It’s about attention. It’s about knowing that 30% less medicine might be the right dose. It’s about listening to the alarms-even the ones you think are wrong.
Every senior deserves to be safe. Not just during a procedure. Not just on paper. But in real time, with real eyes, real hands, and real vigilance.
Can seniors overdose on sedatives even if they’re not on opioids?
Yes. Benzodiazepines like midazolam and zolpidem are common causes of oversedation in seniors. These drugs slow breathing just like opioids. In fact, 37% of overdose cases in patients over 70 involve sedatives alone, not opioids. The same monitoring rules apply: watch breathing rate, use capnography, and use lower doses.
Why is capnography more important than pulse oximetry for seniors?
Pulse oximetry measures oxygen in the blood, but seniors on supplemental oxygen can have normal SpO2 even while holding their breath. Capnography measures carbon dioxide, which builds up when breathing slows. It detects respiratory depression 12-14 minutes before SpO2 drops. For seniors, this early warning is lifesaving.
What is the Richmond Agitation-Sedation Scale (RASS) and how do I use it?
RASS is a 10-point scale from +4 (agitated) to -5 (unarousable). To use it: call the patient’s name. If they don’t respond, gently shake their shoulder. If they open eyes but don’t follow commands, that’s -2 (moderate sedation). If they only move to pain, that’s -4 (deep sedation). A score of -3 or lower means immediate action is needed. Staff should be trained using standardized videos and practice scenarios to ensure consistent scoring.
How often should vital signs be checked during sedation in seniors?
Continuous monitoring is required for heart rate, oxygen saturation, respiratory rate, and end-tidal CO2. Blood pressure should be checked every 5 minutes. Intermittent checks (e.g., every 10 minutes) miss over 75% of dangerous events. The American Society of Anesthesiologists mandates continuous monitoring for all patients over 65 undergoing moderate or deep sedation.
Are there any legal requirements for monitoring seniors during sedation?
Yes. The Joint Commission’s NPSG.02.02.01 requires individualized sedation protocols for high-risk patients, including seniors. Medicare’s Condition of Participation §482.52(c) mandates continuous monitoring of oxygenation, ventilation, and circulation during moderate sedation. Facilities that fail to comply risk losing reimbursement and facing malpractice liability. In 2023, CMS tied 18% of hospital penalties to sedation monitoring failures in elderly patients.





Susan Purney Mark
March 6, 2026 AT 13:50Just wanted to say thank you for this. My mom had a scare last year during a colonoscopy-she was on oxygen, looked fine, but her CO2 was spiking. No one caught it until the alarm went off. 🥲 This post? Lifesaver. I’m sharing it with every family member who’s got an elderly loved one facing sedation.
Tim Hnatko
March 7, 2026 AT 02:59I work in a rural outpatient center. We don’t have capnography. Just oximetry and BP checks every 10 minutes. I’ve been begging admin for months. They say it’s ‘not cost-effective.’ But after reading this, I’m drafting a proposal with the 41% reduction stat from Mayo. Maybe if I show them the numbers, they’ll listen. This isn’t luxury-it’s liability.
Aaron Pace
March 8, 2026 AT 01:35OMG I’m so glad I found this 😍 I’ve been telling my nurse for years that ‘she’s just sleepy’ but now I get it-silent hypoxia is a thing?? Like, my grandma’s on oxygen and she’s ‘fine’ but she hasn’t moved in 20 mins? That’s not nap time. That’s a warning. I’m printing this and taping it to her chart. 💯
Joey Pearson
March 8, 2026 AT 15:46YES. This. Every single word. Start low. Go slow. Watch the monitors. No excuses. If you’re not using capnography on seniors, you’re playing Russian roulette with a loaded gun. 🚨 I’ve seen it happen. Don’t be the one who says ‘I didn’t know.’ You know now.
Weston Potgieter
March 9, 2026 AT 21:07So you’re telling me the whole system is broken? I’ve seen 80-year-olds get full adult doses of fentanyl. They die. They’re not ‘accidents.’ They’re negligence. The fact that this even needs explaining is disgusting. Just do your job. Or stop working with humans.
phyllis bourassa
March 10, 2026 AT 07:40Ugh. Another ‘medical expert’ telling us how to care for our elders. You know what’s worse than oversedation? Being treated like a statistic. My aunt’s not a ‘case study.’ She’s a woman who loved jazz and hated broccoli. Maybe if you spent less time quoting studies and more time holding her hand, you’d understand why she’s scared.
Ferdinand Aton
March 12, 2026 AT 05:05Actually, capnography is overrated. In my 15 years in ICU, I’ve seen more false positives than real alarms. Sometimes the machine glitches. Sometimes the patient just has a weird breathing pattern. You can’t just trust tech. Experience matters more than numbers.
William Minks
March 12, 2026 AT 22:27I’m from rural Kenya, and we don’t have capnography machines. We use observation. Pulse, breath, color, response. It’s not perfect, but it’s human. Maybe we need to trust the caregiver’s intuition more than the monitor. Sometimes the quietest ones are the ones who need the most attention.
Jeff Mirisola
March 14, 2026 AT 16:19This is brilliant. I’ve been pushing for IPI monitors in our ER for months. We just got our first two last week. One of our 83-year-old patients had a drop to 5.8 during a procedure. We paused. He woke up 2 minutes later. No harm. This isn’t just theory-it’s saving lives right now. Thank you for giving us the language to fight for this.
Ian Kiplagat
March 15, 2026 AT 09:18Agreed. Continuous monitoring is non-negotiable. But let’s not forget: the most important tool is still the nurse who’s actually in the room. Not the machine. Not the protocol. The person who notices the slight shift in breathing. The one who leans in. That’s what saves lives.
Roland Silber
March 16, 2026 AT 02:38Just wanted to add something: the 0.5% per year formula is great, but it’s not universal. Frailty matters more than age. A healthy 80-year-old might handle 80% of the standard dose. A 70-year-old with COPD and kidney disease might need 40%. Always assess function, not just birth year. I use the Clinical Frailty Scale alongside the formula. It’s changed how I dose. Also-never forget to ask the patient’s family what’s normal for them. Sometimes the ‘agitated’ behavior is just their way of saying ‘I’m scared.’
And yes, IPI is magic. We started using it last month. Our oversedation rate dropped 52%. Staff are now trained to respond to IPI < 7 like it’s a code blue. No hesitation. No ‘let’s wait and see.’ If it’s below 7, you stop. Period.
One more thing: hydrocolloid dressings for RVM? Lifesaver. We use 3M Tegaderm + a thin layer of Duoderm. Electrodes stay on for 12+ hours. No more reapplying every 20 minutes. Small change. Huge difference.