Reading the label on your extended-release medication isn’t just about following instructions-it’s about staying safe. These pills aren’t like regular tablets. If you crush, split, or take them at the wrong time, you could end up with too much medicine in your system all at once. That’s not a small risk. Between 2018 and 2022, over 1,200 adverse events were reported to the FDA just from people mishandling extended-release drugs. One person crushed OxyContin and ended up in the ICU. Another took Adderall XR at night and stayed awake for 36 hours. This isn’t rare. Pharmacists report seeing 2-3 cases like this every month.
What Does "Extended-Release" Actually Mean?
Extended-release (ER, XR, SR, CR, CD) means the medicine is built to release slowly over time. Instead of your body absorbing the full dose right away, it gets a steady trickle over 12 or 24 hours. This helps keep your blood levels steady so you don’t have spikes or crashes. It also means you only need to take it once or twice a day instead of every 6-8 hours. For example, a regular diltiazem tablet might need three doses daily. The extended-release version, like Cardizem CD or Taztia XT, works for a full 24 hours with just one pill.
But here’s the catch: different brands use different ways to make this happen. Some use a polymer coating that dissolves slowly. Others mix the drug into a gel-like matrix that breaks down over time. Concerta, for instance, uses an osmotic system that pushes the drug out through a tiny hole. If you crush it, you destroy the whole mechanism. The label might say "extended release" on all of them, but they’re not the same.
How to Spot Extended-Release on the Label
Look for these suffixes right after the drug name:
- ER - Extended Release
- XR - eXtended Release
- SR - Sustained Release
- CR - Controlled Release
- CD - Continuous Delivery
Also check for phrases like "24 hour" or "12 hour" right after the release type. For example: "Metoprolol succinate 24 hour extended release [Toprol XL] 25 mg". The "24 hour" part is critical. A 12-hour version will need two doses a day. A 24-hour version only needs one.
Don’t assume "extended release" means "longer-lasting effect". That’s what many older adults think, according to a 2022 FDA study. But it doesn’t tell you how the drug works. The real clue is the brand name in parentheses. If you see "[Toprol XL]" or "[Concerta]", those are proprietary systems. Generic versions might look similar but work differently.
What the Label Tells You (And What It Doesn’t)
On prescription labels, look for three key sections:
- Directions: This tells you when to take it. "Take once daily in the morning" or "Take at bedtime" matters. Niaspan, for example, causes flushing if taken during the day. Taking it at night reduces that side effect.
- Warnings: This is non-negotiable. It will say: "DO NOT CRUSH, SPLIT, OR CHEW." This isn’t a suggestion. It’s a safety rule. Crushing an extended-release tablet releases the full dose instantly. That’s like taking four pills at once.
- Inactive Ingredients: These are the fillers and coatings. While not active, they’re part of how the drug releases. Some people are sensitive to dyes or preservatives in the coating.
On over-the-counter (OTC) meds, the Drug Facts panel (required since 2017) has the same info. If you’re using Aleve PM or a similar product, the label will say "extended-release" but usually won’t specify 12 vs. 24 hours. In those cases, follow the dosing schedule exactly as written.
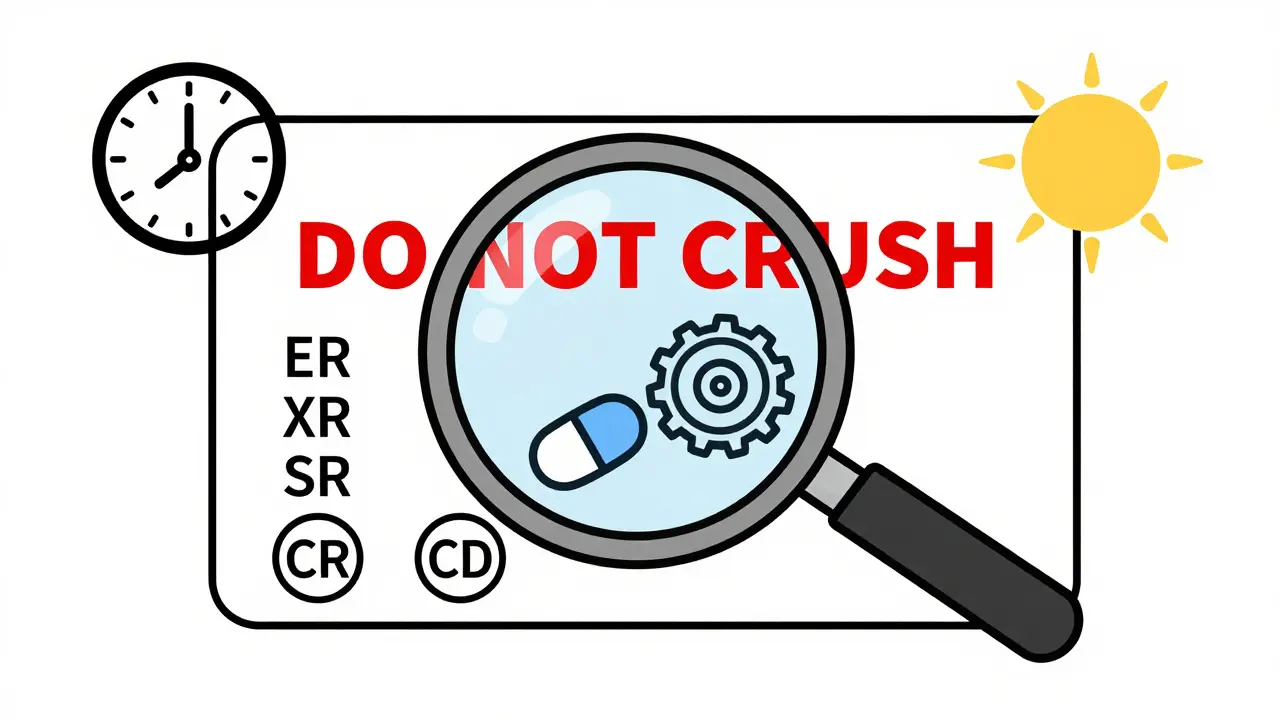
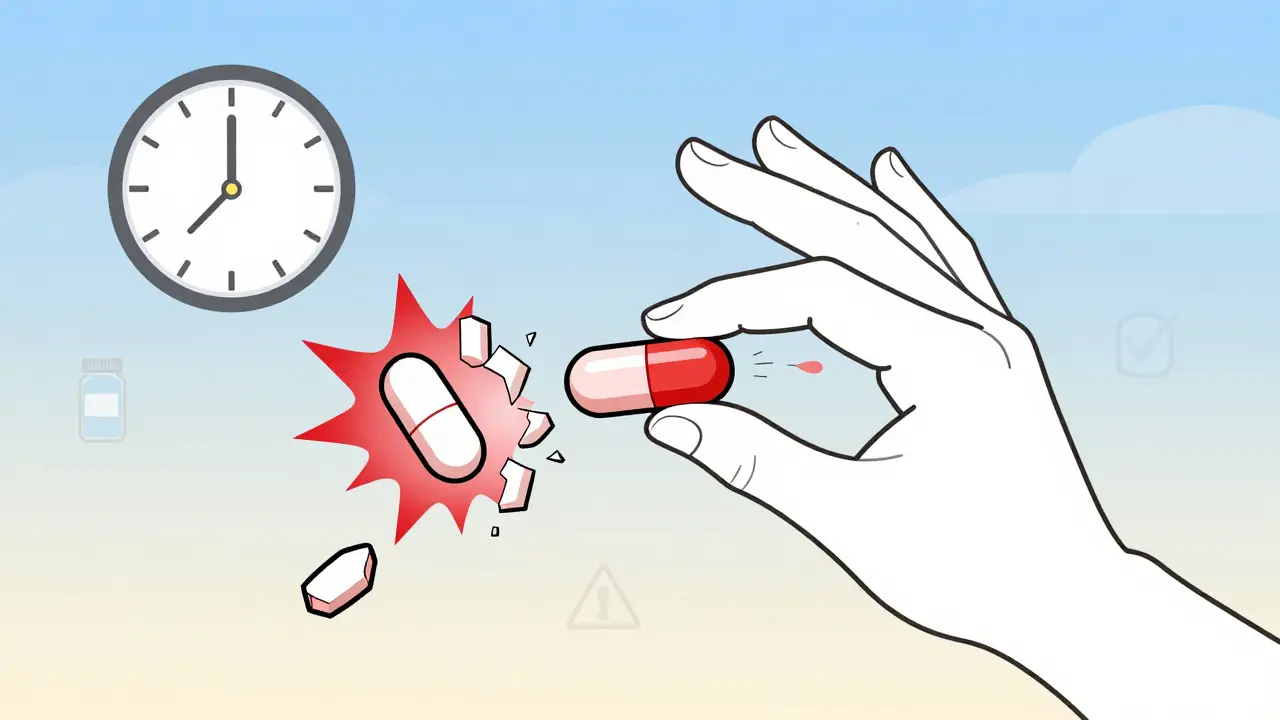
Why You Can’t Just Crush or Split Them
Imagine a time-release capsule like a slow-drip water bottle. If you break it open, all the water gushes out at once. That’s what happens with these medications. Crushing or splitting an extended-release pill can cause:
- A sudden spike in drug levels
- Toxic overdose
- Heart rhythm problems
- Respiratory depression (especially with opioids)
One patient crushed 60 mg of OxyContin and snorted it. The entire dose hit their system in seconds. They survived, but barely. Another person split a 24-hour metformin tablet thinking it would stretch the dose. Instead, they had severe diarrhea and low blood sugar for days.
The FDA’s 2023 update now requires all new extended-release labels to have high-contrast "DO NOT CRUSH" warnings. If your label doesn’t have it, ask your pharmacist. Older prescriptions might still be out there.
Timing Matters More Than You Think
Some extended-release meds work best at specific times. Here are real examples:
- Niaspan (niacin): Take at bedtime to reduce flushing.
- Propranolol ER: Take in the morning to avoid nighttime low blood pressure.
- Metformin XR: Take with dinner to reduce stomach upset.
- Concerta: Take in the morning. It can interfere with sleep if taken later.
One user on Drugs.com wrote: "I took Adderall XR at night because I thought it would last all day. I didn’t sleep for 36 hours." That’s not a side effect-it’s a mistake in timing. The label didn’t say "take anytime." It said "take in the morning." That’s not arbitrary. It’s science.
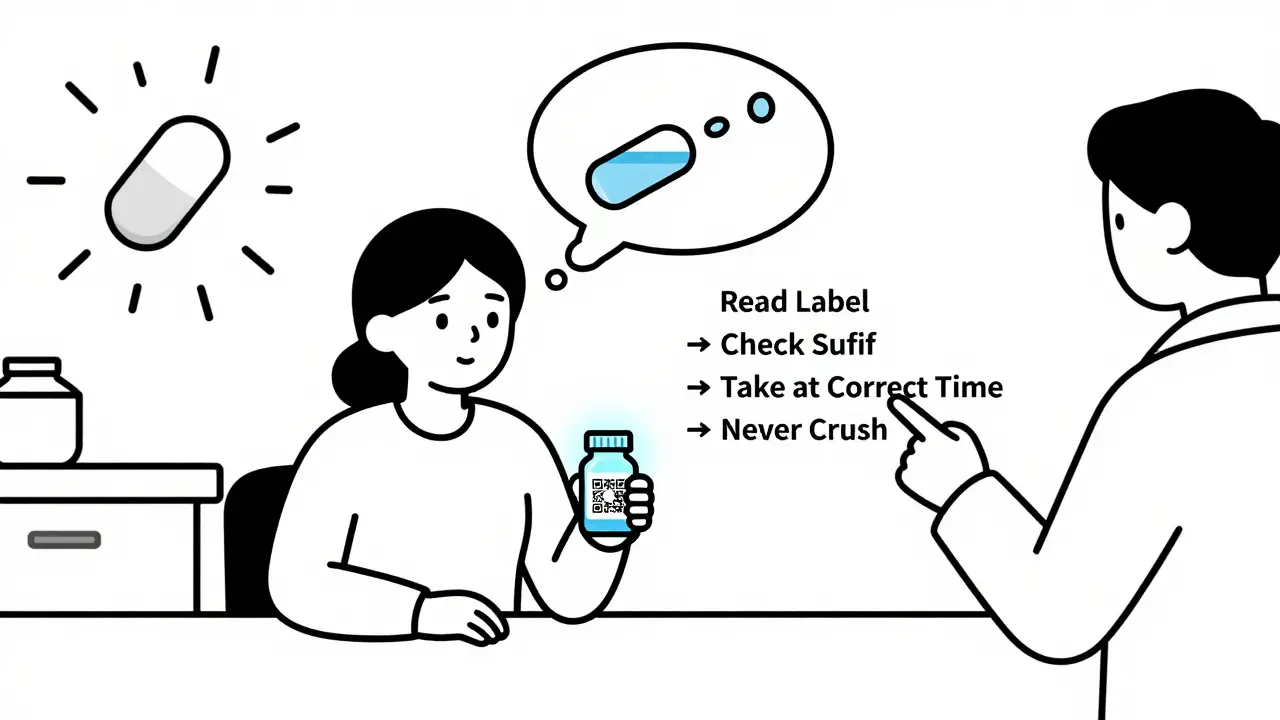
What to Do If You’re Confused
Don’t guess. Don’t assume. Don’t rely on memory.
Here’s what to do instead:
- Ask your pharmacist. Say: "Can you explain how this extended-release version works?" They’re trained to break it down.
- Use the teach-back method. After they explain, say: "So, I take this once a day in the morning, and I can’t crush it, right?" If they nod, you got it.
- Check for QR codes. Newer labels have them. Scan with your phone. It might play a 30-second video showing how to take the pill.
- Download the Medication Guide. The FDA requires these for high-risk drugs. They’re printed and given to you. If you didn’t get one, ask for it.
Also, don’t assume two pills with the same name work the same. For example, there are three different 24-hour versions of diltiazem. They’re not interchangeable. One might work better for you than another. Your doctor picked one for a reason. Don’t swap them without talking to them.
What’s Changing in 2026
The rules are getting stricter. Starting in 2024, all new extended-release drugs must have "24 hour extended release" written out fully-not just "ER" or "XR". This is to stop confusion. In digital prescriptions, EHR systems now require the full phrase too.
Also, new technologies are coming. Some pills now use GI retention systems that can last 48-72 hours. These aren’t common yet, but they’re on the horizon. The label will change again. The key is to always read the label, every time you refill.
Extended-release meds are a huge help for people managing chronic conditions. One patient with multiple sclerosis said switching to Gilenya’s once-daily dose raised her adherence from 62% to 98%. That’s life-changing. But only if you take it right.
Final Reminder
Extended-release doesn’t mean "stronger." It means "slower."
Don’t crush. Don’t split. Don’t skip doses. Don’t change the time. And if you’re unsure-ask. Always.
Can I cut an extended-release pill in half if I can’t swallow it whole?
No. Cutting, crushing, or chewing an extended-release pill destroys its slow-release mechanism. This can release the entire dose at once, leading to overdose. If you have trouble swallowing pills, ask your pharmacist or doctor for an alternative form-like a liquid, patch, or capsule that can be opened (only if approved). Never assume a pill is safe to split just because it looks like it has a score line.
Why do some extended-release pills have different names even if they contain the same drug?
Different brands use different technologies to release the drug. For example, Concerta uses an osmotic pump system, while generic versions often use a matrix system. Even though both are labeled "extended release," they release the drug at different rates. The FDA doesn’t consider them interchangeable. Always take the exact brand and formulation your doctor prescribed. Switching without approval can change how well the medicine works or increase side effects.
Is it okay to take an extended-release medication with food?
It depends. Some extended-release pills work better with food, like metformin XR, which is taken with dinner to reduce stomach upset. Others, like certain blood pressure meds, should be taken on an empty stomach. Always check the label or ask your pharmacist. Food can affect how quickly the drug is absorbed, which can change its effectiveness or increase side effects.
What should I do if I miss a dose of my extended-release medication?
If you miss a dose, don’t double up. Most extended-release meds are designed to be taken once daily. If you remember within a few hours of your usual time, take it then. If it’s almost time for your next dose, skip the missed one and go back to your regular schedule. Never take two doses at once. Doing so could cause a dangerous spike in drug levels. If you’re unsure, call your pharmacist.
Are extended-release medications more expensive?
Yes, they usually cost 20-35% more than immediate-release versions. But they can save money in the long run by reducing hospital visits. A 2022 study found patients on extended-release meds had 18-22% fewer hospitalizations because they took their pills more consistently. If cost is an issue, ask your pharmacist about generic options. Some generics work just as well-but only if they’re the same formulation as your original prescription.





Kenneth Jones
March 23, 2026 AT 11:46Grace Kusta Nasralla
March 23, 2026 AT 17:41Korn Deno
March 24, 2026 AT 13:17Aaron Sims
March 25, 2026 AT 23:25Stephen Alabi
March 27, 2026 AT 20:39Agbogla Bischof
March 28, 2026 AT 15:18Pat Fur
March 29, 2026 AT 00:25Anil Arekar
March 29, 2026 AT 14:40Elaine Parra
March 30, 2026 AT 21:29Natasha Rodríguez Lara
March 31, 2026 AT 15:44Amber Gray
March 31, 2026 AT 22:04Danielle Arnold
April 1, 2026 AT 18:48James Moreau
April 1, 2026 AT 18:50