Perioperative Anticoagulant Timing Calculator
Calculate Safe Anticoagulant Timing
Results
Enter your procedure details to see safe timing recommendations.
Why Stopping Blood Thinners Before Surgery Isn’t One-Size-Fits-All
Imagine you’re scheduled for knee replacement surgery. You’ve been taking apixaban for atrial fibrillation for two years. Your surgeon says, "Stop your blood thinner." But when? How long? Should you get a bridge shot of heparin? If you guess wrong, you could bleed out on the table-or suffer a stroke days later. This isn’t hypothetical. Around 17% to 23% of patients on direct oral anticoagulants (DOACs) experience major bleeding during emergency surgeries, according to 2024 data from the American College of Cardiology. At the same time, 7% to 16% face a blood clot if anticoagulation is stopped too long. The goal isn’t to stop the medicine-it’s to time it right.
DOACs vs. Warfarin: Two Different Rules
Not all blood thinners are the same. Warfarin, the old-school option, takes days to clear from your system. You stop it five days before surgery and check your INR level to make sure it’s below 1.5. You might even get heparin shots in between to prevent clots-though that’s becoming rare.
DOACs like apixaban, rivaroxaban, dabigatran, and edoxaban are different. They leave your body in hours, not days. Rivaroxaban clears in 5 to 9 hours. Apixaban in 8 to 15. That’s why you don’t need heparin bridging for most people anymore. The PAUSE study in 2018 proved it: stopping DOACs for 2 to 4 days before surgery and restarting them 1 to 3 days after, with no bridge, was just as safe as bridging-and far less likely to cause bleeding.
Here’s the breakdown:
- Apixaban, rivaroxaban, edoxaban: Stop 3 days before surgery. Restart 24 to 72 hours after, depending on bleeding risk.
- Dabigatran: Stop 4 days before surgery. Restart same as others.
- Warfarin: Stop 5 days before. Restart 12 to 24 hours after if bleeding is controlled.
These aren’t suggestions. They’re based on large, real-world studies. Skipping the bridge cuts major bleeding risk by nearly half in low-to-moderate thrombosis risk patients.
When Bridging Still Makes Sense (And When It Doesn’t)
For years, doctors gave heparin shots to patients stopping warfarin, thinking it prevented clots. Now we know better. The 2022 American Society of Hematology guidelines say: Don’t bridge for DOACs. Ever. The risk of bleeding outweighs any tiny theoretical benefit.
Even for warfarin, bridging is now limited to high-risk cases. That means patients with:
- Mechanical mitral valves
- Recent venous thromboembolism (VTE) in the last 3 months
- History of stroke from atrial fibrillation within the past year
For everyone else-especially those with atrial fibrillation and a CHA2DS2-VASc score of 2 or higher-stopping the DOAC for 3 to 4 days carries less than a 0.1% risk of stroke. That’s lower than the chance of getting hit by lightning. Bridging adds bleeding risk without reducing stroke risk.
And here’s the kicker: even for mechanical valves, the 2023 CHEST guidelines now say to suggest against bridging. Many hospitals still do it out of habit. But the evidence is clear: no benefit. More bleeding.
Neuraxial Anesthesia: The One Exception That Demands Precision
If you’re getting an epidural or spinal block, the rules tighten. A spinal hematoma can paralyze you. That’s why ASRA guidelines are strict:
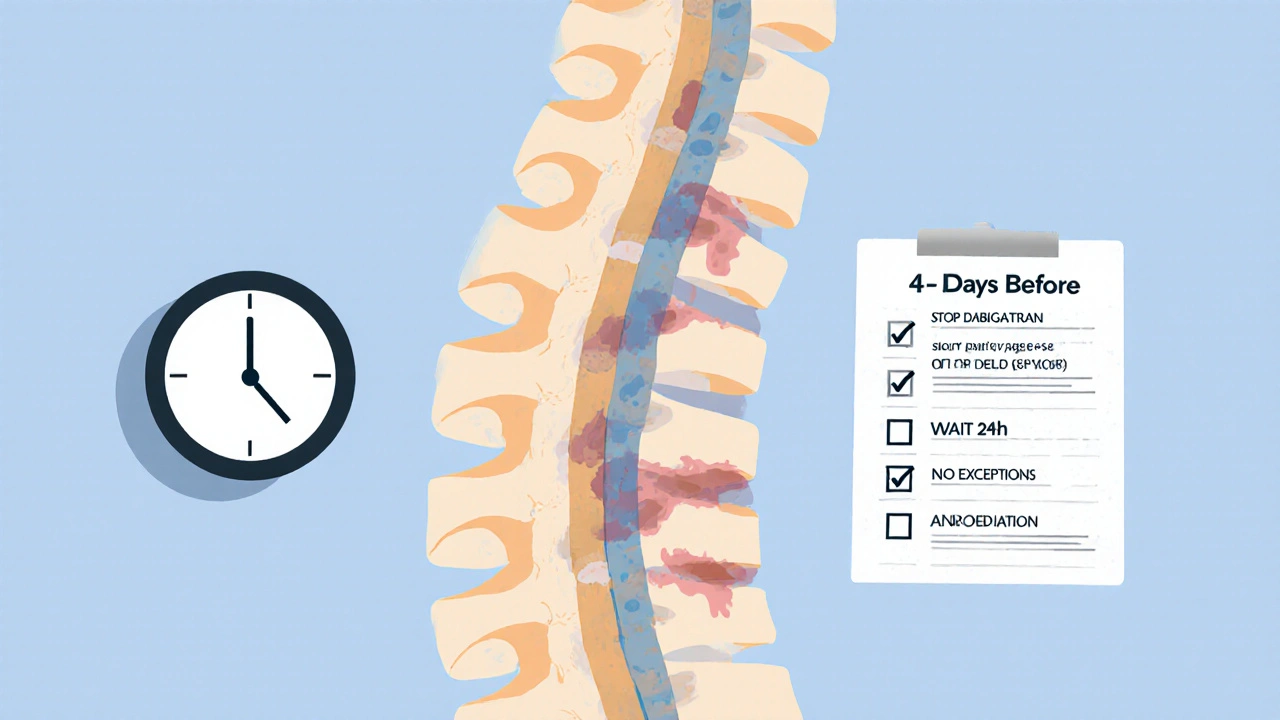
- Stop apixaban, rivaroxaban, edoxaban: 3 full days before
- Stop dabigatran: 4 full days before
- Wait at least 24 hours after surgery before restarting
There’s no wiggle room. No shortcuts. No "I think it’s safe." The 2023 Anesthesia & Analgesia editorial from Dr. Jerrold H. Levy says it plainly: timing here is non-negotiable. Even a 12-hour delay in stopping can be dangerous. That’s why anesthesiologists now check your last dose time like a flight log. No exceptions.

What About Emergencies? Reversal Agents and Their Costs
What if you need emergency surgery and you’re still on your blood thinner? That’s when reversal agents come in. But they’re expensive and risky.
- Idarucizumab (Praxbind): Reverses dabigatran. One 5g vial costs $3,700. Works in minutes.
- Andexanet alfa (Andexxa): Reverses factor Xa inhibitors (apixaban, rivaroxaban, etc.). One dose is $19,000. Works fast-but 13% of patients in trials had a stroke afterward.
The ANNEXA-4 and RE-VERSE AD trials showed these drugs work to stop bleeding. But they also bring back clotting risk. Andexanet alfa caused thrombotic events in 18% of patients within 30 days. That’s why doctors only use them when bleeding is life-threatening. They’re not a safety net. They’re a last resort.
Know Your Scores: CHA2DS2-VASc and HAS-BLED
Doctors don’t guess. They use scores. Two matter most:
- CHA2DS2-VASc: Measures stroke risk in atrial fibrillation. Points for age, heart failure, hypertension, diabetes, prior stroke, vascular disease, female sex. Score of 2 or higher? You’re at risk. But even then, a 3- to 4-day break from DOACs is safe.
- HAS-BLED: Measures bleeding risk. Points for high blood pressure, liver or kidney disease, stroke history, labile INR, elderly, drugs like aspirin, alcohol abuse. Score of 3 or higher? You’re at higher bleeding risk. That doesn’t mean stop anticoagulation-it means be extra careful with timing and resumption.
According to the 2023 ACC, misapplying these scores leads to 32% of wrong anticoagulation decisions. That’s not a small error. It’s a systemic problem. If your doctor doesn’t run these scores, ask why.
Low-Risk Procedures: You Might Not Need to Stop at All
Not every surgery requires stopping your blood thinner. For low-bleeding-risk procedures, you can often keep taking it:
- Cataract surgery
- Dental extractions (with local anesthesia)
- Biopsies (skin, breast)
- Minor skin surgeries
- Colonoscopies with no polyp removal
Studies show bleeding risk is minimal. Stopping increases clot risk without benefit. The 2023 AAFP guidelines back this up. If your surgeon says, "Stop everything," ask if your procedure is truly high-risk. Many don’t know the difference.
Resuming After Surgery: Don’t Wait Too Long
Stopping is only half the battle. Restarting matters just as much. Delaying anticoagulation too long raises clot risk. The PAUSE study showed restarting DOACs within 24 to 72 hours after surgery-depending on bleeding risk-was safe.
Here’s the logic:
- Low bleeding risk surgery (e.g., hernia repair): Restart DOAC at 24 hours.
- High bleeding risk surgery (e.g., brain tumor removal): Wait 72 hours. Start with prophylactic dose if needed.
Don’t wait until day 5. Your body starts forming clots within 48 hours after major surgery. Waiting too long is like leaving the door open.
The Big Picture: Why This Matters More Than Ever
Over 15 million Americans take anticoagulants. Half of them will need surgery in their lifetime. The National Surgical Quality Improvement Program (NSQIP) found that improper anticoagulation management causes 8.7% of preventable surgical complications. That’s tens of thousands of avoidable bleeds and strokes every year.
But progress is real. A 2022 JAMA study of 45 academic hospitals showed 89% now follow DOAC discontinuation guidelines. Only 63% get the restart right. That’s the gap. That’s where patients still get hurt.
The future is coming. Ciraparantag, a universal reversal agent now in Phase 3 trials, could reverse all anticoagulants in under 10 minutes. But even then, the core principle won’t change: match the interruption to the risk. Not the drug. Not the habit. Not the fear. The risk.
What You Should Do Before Your Surgery
- Know your drug: Is it a DOAC or warfarin?
- Know your score: Ask for your CHA2DS2-VASc and HAS-BLED scores.
- Know your procedure: Is it high or low bleeding risk? Ask your surgeon.
- Know the plan: Get written instructions on when to stop and restart. Don’t rely on memory.
- Ask: "Will I need heparin bridging?" If yes, ask why-based on current guidelines.
Most patients are scared to question their doctors. But this isn’t about being difficult. It’s about being safe. Your life depends on the timing of a pill.





Adam Hainsfurther
November 25, 2025 AT 00:24Rachael Gallagher
November 25, 2025 AT 11:05steven patiño palacio
November 25, 2025 AT 16:14stephanie Hill
November 26, 2025 AT 13:51Akash Chopda
November 28, 2025 AT 02:40Nikki C
November 29, 2025 AT 00:38Alex Dubrovin
November 29, 2025 AT 12:47Jacob McConaghy
December 1, 2025 AT 02:30Natashia Luu
December 1, 2025 AT 19:14akhilesh jha
December 3, 2025 AT 08:06Jeff Hicken
December 3, 2025 AT 11:20Vineeta Puri
December 5, 2025 AT 01:56