Medication Interaction Risk Calculator
Your risk of adverse drug events increases with the number of medications you take. Based on clinical studies, this calculator shows how your risk compares to someone taking just one medication.
Every year, thousands of people end up in the hospital not because their medication didn’t work, but because it worked too well-or in the wrong way. A common painkiller taken with an antibiotic. Grapefruit juice with a cholesterol drug. A supplement mixed with an antidepressant. These aren’t rare mistakes. They’re preventable drug interactions that turn mild side effects into life-threatening emergencies.
What Happens When Drugs Clash?
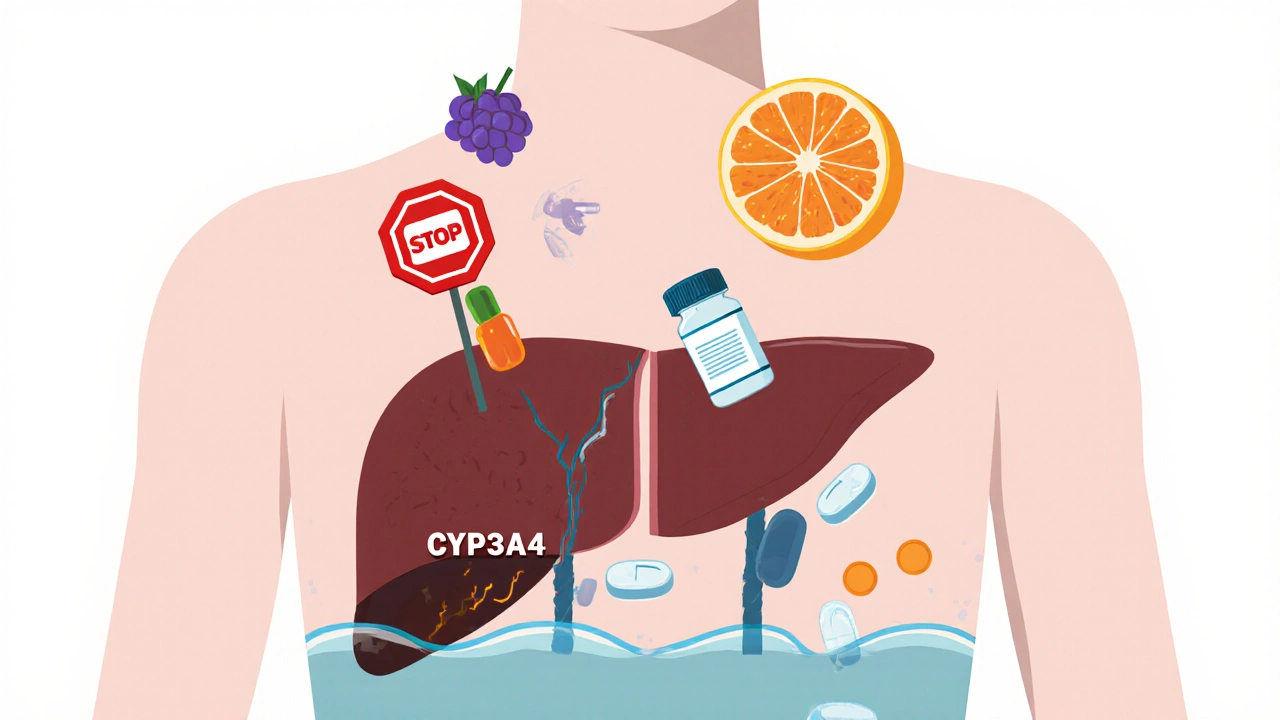
Your body doesn’t treat every drug like a separate guest at a party. It treats them like competitors fighting for the same doorway. When two or more drugs enter your system, they can block, boost, or confuse each other’s path through your liver, kidneys, and bloodstream. This is called a drug interaction. And it’s not just about pills. It’s about food, supplements, even your genes. The most dangerous interactions happen because of something called the cytochrome P450 system-specifically, the CYP3A4 enzyme. This enzyme is responsible for breaking down about half of all prescription medications. When another drug shuts it down-like clarithromycin, ketoconazole, or even grapefruit juice-the first drug doesn’t get broken down. It builds up. And that buildup? That’s what turns dizziness into fainting, muscle aches into rhabdomyolysis, or a slight increase in bleeding into a stroke. Take statins. They’re safe for most people. But when combined with a CYP3A4 inhibitor, the risk of muscle damage jumps 8.4 times. In one study, patients on simvastatin with clarithromycin had 2.7 cases of rhabdomyolysis per 10,000. With azithromycin-which doesn’t interfere-that number dropped to 0.3. That’s a 90% reduction in risk just by switching antibiotics.Why Some People Are at Higher Risk
Not everyone reacts the same way. Your genes play a huge role. About 3 to 10% of people of European descent have a genetic variation that makes them poor metabolizers of CYP2D6. That means drugs like codeine, tramadol, or certain antidepressants stay in their system way too long. One person might get pain relief from codeine. Another, with the same prescription, could overdose on morphine-because their body converts codeine to morphine too slowly, then suddenly floods the system with it. Older adults are another high-risk group. On average, they take five or more medications. Studies show that people on five or more drugs have a 78% higher chance of an adverse drug event. Those on ten or more? Their risk jumps 153%. It’s not just the number of pills. It’s the combinations. Warfarin, for example, interacts with over 100 drugs. Add amiodarone? Bleeding risk goes up 2.5 times. Take too much acetaminophen? That also spikes bleeding risk. And no one tells you that.
Food, Supplements, and the Hidden Triggers
You’ve heard not to drink grapefruit juice with statins. But did you know it doesn’t affect all statins the same way? Grapefruit juice increases felodipine levels by 300%. With amlodipine? Just 15%. That’s why some doctors will switch you to a different drug-not because the first one didn’t work, but because your diet was quietly sabotaging it. Vitamin K is another sneaky player. If you’re on warfarin, your blood thinning depends on your vitamin K intake being steady. One week you eat a big salad. Next week, you skip it. Your INR level drops. Your doctor thinks the warfarin stopped working. It didn’t. Your diet did. Supplements are even worse. St. John’s wort, a popular herbal remedy for depression, can reduce the effectiveness of birth control pills, blood thinners, and even some cancer drugs by up to 50%. People take it because it’s “natural.” But “natural” doesn’t mean safe-especially when mixed with prescription meds.What Doctors Miss (And What Nurses See)
A 2022 study across 12 hospitals found that 68% of hospitalized patients had at least one drug interaction. Nurses caught 40% of these that doctors missed. Why? Doctors are overwhelmed. A 2023 survey of 3,500 physicians showed that 74% felt buried under drug interaction alerts. And here’s the kicker: 90 to 95% of those alerts in electronic health records are low-risk. They’re noise. So doctors start ignoring them. That’s called alert fatigue. And it’s deadly. Only 7% of alerts are for high-risk interactions. But when you’re flooded with 50 warnings a shift, you stop reading them. Patients pay the price. Reddit threads from r/pharmacy in 2023 had 147 verified stories: muscle pain from statins + grapefruit, serotonin syndrome from SSRIs + tramadol, unstable INR from warfarin + vitamin K. These aren’t outliers. They’re predictable.
How to Protect Yourself
You don’t need to be a pharmacist to avoid dangerous interactions. Here’s what actually works:- Keep a full list of everything you take-prescriptions, over-the-counter meds, vitamins, herbs, even occasional painkillers. Bring it to every appointment.
- Ask your pharmacist when you pick up a new prescription: “Could this interact with anything else I’m taking?” Pharmacists are trained for this. They catch what doctors miss.
- Use a single pharmacy. If you get your meds from different places, no one sees the full picture. One pharmacy can flag dangerous combinations.
- Check grapefruit juice warnings. If your pill says “avoid grapefruit,” it’s not a suggestion. It’s a warning. Switch to orange juice instead.
- Don’t start supplements without asking. Even “safe” ones like fish oil or magnesium can interfere with blood pressure or heart meds.
The Future: Smarter Tools, Fewer Mistakes
The good news? We’re getting better at stopping this. AI models now predict dangerous interactions with 89% accuracy-22% better than old systems. Some hospitals are using pharmacogenetic testing to tailor prescriptions based on your genes. In pilot programs, this cut high-risk interactions by 36%. New tools are also being tested: wearable sensors that monitor drug levels in real time, and blockchain systems that share your full medication history between clinics. Right now, 87% of U.S. hospitals use electronic interaction checkers. But only 32% have pharmacists actively reviewing high-risk patients’ meds. That’s the gap. The bottom line? Drug interactions aren’t accidents. They’re system failures. And they’re preventable. With better tools, better training, and better communication, we could stop 150,000 to 200,000 serious adverse events every year in the U.S. alone.It’s not about avoiding medicine. It’s about using it wisely. Your next pill might save your life. But if it’s mixed with the wrong thing, it could end it.
Can over-the-counter drugs cause dangerous interactions?
Yes. Common OTC drugs like ibuprofen, naproxen, and even antacids can interact with prescription meds. Ibuprofen with warfarin increases bleeding risk. Antacids with antibiotics like tetracycline can block absorption by up to 90%. Even allergy meds like diphenhydramine can worsen drowsiness when mixed with opioids or benzodiazepines.
Are natural supplements safer than prescription drugs?
No. Supplements aren’t regulated like drugs, so their strength and ingredients can vary. St. John’s wort, garlic, ginkgo, and goldenseal all interfere with blood thinners, antidepressants, and transplant meds. Just because it’s sold in a health food store doesn’t mean it’s safe with your prescriptions.
Why do some drug interactions happen even if I take my meds at different times?
Because the problem isn’t timing-it’s chemistry. Some drugs stay in your system for days. Grapefruit juice can inhibit CYP3A4 for up to 72 hours. So even if you take your statin in the morning and grapefruit juice at night, the enzyme is still blocked. The body doesn’t reset quickly enough to avoid the interaction.
Can my genetics make me more prone to drug interactions?
Absolutely. About 3-10% of people have genetic variants that make them poor metabolizers of key enzymes like CYP2D6 or CYP2C19. That means drugs like codeine, clopidogrel, or certain antidepressants build up to toxic levels. Pharmacogenetic testing can identify these risks before you even start a new medication.
What should I do if I think I’m having a drug interaction?
Stop taking the new medication or supplement immediately, and call your doctor or pharmacist. Don’t wait. Symptoms like unusual bruising, muscle pain, confusion, rapid heartbeat, or severe dizziness could signal a dangerous interaction. Keep a list of everything you took and when-this helps them diagnose the issue faster.
How often should I review my medications?
At least once a year, or anytime you start or stop a medication-even if it’s just a short-term antibiotic or a new pain reliever. Many interactions happen after a hospital stay or when a new doctor prescribes something without knowing your full history. A full medication review with your pharmacist can cut your risk of adverse events by up to 30%.



Jack Riley
November 24, 2025 AT 21:06So let me get this straight - we’re all just guinea pigs in a pharmaceutical circus where the ringmaster is a pharmacist who hasn’t slept since 2019? I take aspirin for my headache, grapefruit juice for my ‘detox,’ and St. John’s wort because my cousin swears it’s ‘better than Prozac’ - and somehow I’m supposed to survive this? The system isn’t broken. It’s a haunted house with a pharmacy logo on the door.
Jacqueline Aslet
November 26, 2025 AT 15:34It is, without question, an egregious failure of systemic medical oversight that patients are left to navigate pharmacological minefields with the cognitive bandwidth of a distracted squirrel. The proliferation of polypharmacy, coupled with the absence of coordinated care protocols, constitutes a profound dereliction of professional duty. One must wonder whether the commodification of healthcare has rendered human life a secondary consideration.
Caroline Marchetta
November 27, 2025 AT 17:37Oh wow. So now we’re supposed to be *careful*? I mean, I guess I should’ve known that my ‘natural’ turmeric capsules were quietly turning my blood into soup. But hey - at least I’m not on 12 meds like my neighbor who takes a pill for the pill she took to stop the side effect of the other pill. 🙃
Valérie Siébert
November 29, 2025 AT 09:55YOOO I JUST REALIZED I’VE BEEN TAKING MAGNESIUM WITH MY BP MED AND NOW I’M PANICKING 😭 I THOUGHT IT WAS ‘SAFE’ BECAUSE IT’S IN BANANAS??!!? CAN SOMEONE TELL ME IF I’M GONNA DIIIE??
katia dagenais
November 30, 2025 AT 06:22Let’s be real - the whole thing is a scam. Big Pharma doesn’t want you to know that 90% of these ‘interactions’ are just profit-driven noise. They push 50 different statins, each with its own grapefruit warning, so you keep buying new ones. Meanwhile, the real solution? Stop eating processed food, sleep more, and stop taking 17 supplements because ‘your gut needs help.’ But that’s not profitable, is it? 😏
Josh Gonzales
December 1, 2025 AT 03:54My grandma takes 8 meds and a bunch of herbs. She doesn’t know half of what they do. Her pharmacist caught three dangerous combos last year. He’s the real MVP. Doctors are busy. Pharmacists are the ones who actually read the labels. Go to one pharmacy. Keep a list. Ask questions. It’s not hard. It’s just not taught.
Timothy Sadleir
December 1, 2025 AT 06:18And yet the CDC, FDA, and every major hospital are complicit in this. The truth? The entire pharmaceutical-industrial complex is designed to keep you medicated, confused, and dependent. They don’t want you cured. They want you on lifelong maintenance. That’s why they suppress natural alternatives. That’s why they bury the data on drug interactions. Wake up. This isn’t medicine. It’s control.
Jennifer Griffith
December 2, 2025 AT 05:01okay but like… why is grapefruit juice the villain again? i mean, i get that it messes with enzymes but… what if i just dont drink it? why is this even a thing? also why do people take st. john’s wort? it tastes like regret.
Roscoe Howard
December 2, 2025 AT 12:00Let’s not pretend this is just about science. This is a cultural collapse. In America, we treat medication like candy. We pop pills like they’re Skittles. We don’t respect the body. We don’t respect the science. We just want a quick fix. Meanwhile, in countries with real healthcare, people don’t need 12 drugs. They eat real food, move, and let their bodies heal. We’ve become a nation of chemical zombies.
Lisa Odence
December 2, 2025 AT 17:42OMG I JUST REALIZED I’VE BEEN DRINKING GRAPEFRUIT JUICE WITH MY SIMVASTATIN FOR 3 YEARS 😭😭😭 I’M GOING TO DIE AND NO ONE WILL CARE 😭 I’M SO SAD AND I JUST WANTED TO FEEL HEALTHY 😭
Agastya Shukla
December 3, 2025 AT 22:35In India, we’ve always had the practice of consulting Ayurvedic practitioners before combining herbs with allopathic drugs. It’s not perfect, but there’s awareness. Here, the disconnect between traditional knowledge and modern pharmacology is staggering. We need bridges, not walls. A patient shouldn’t have to be a pharmacologist to stay alive.
Aki Jones
December 4, 2025 AT 21:29They’re watching you. The NSA, the FDA, the pharmaceutical CEOs - they know you’re taking grapefruit juice with your statin. They’ve been tracking your pharmacy logs since 2017. The ‘alert fatigue’? It’s not an accident. It’s a deliberate design to let you die quietly. The system doesn’t want you to survive. It wants you to be a statistic. You’re not a patient. You’re a data point.
Elise Lakey
December 6, 2025 AT 14:22This was so helpful. I’ve been terrified to ask my doctor about my supplements, but now I’m going to bring my list to my next appointment. I used to think I was being paranoid. Turns out, I was just smart. Thank you for writing this. You made me feel less alone.
Sharley Agarwal
December 7, 2025 AT 03:14St. John’s wort is a scam. Don’t take it. Just cry harder.
prasad gaude
December 8, 2025 AT 11:55Back home in Kerala, my aunty says: ‘If you want to heal, don’t chase the pill - chase the silence.’ She means rest. Sunlight. Quiet meals. No phones. No supplements. No fear. Maybe the real interaction isn’t between drugs… it’s between us and our own bodies. We forgot how to listen.